Case management in Facilities
Date: 19 March 2020 Source: WHO
WHO continues to monitor the situation closely for any changes that may affect this interim guidance. Should any factors change, WHO will issue a further update. Otherwise, this interim guidance document will expire 2 years after the date of publication.
© World Health Organization 2020. Some rights reserved. This work is available under the CC BY-NC-SA 3.0 IGO licence.
WHO reference number: WHO/2019-nCoV/HCF_operations/2020.1
Contents
Background
This document is intended for health ministers, health system administrators, and other decision-makers. It is meant to guide the care of COVID-19 patients as the response capacity of health systems is challenged; to ensure that COVID-19 patients can access life-saving treatment, without compromising public health objectives and safety of health workers. It promotes two key messages:
- Key public health interventions regardless of transmission scenario; and
- Key action steps to be taken by transmission scenario to enable timely surge of clinical operations.
The public health objectives at all stages of the preparedness and response plan are to:
- Prevent outbreaks, delay spread, slow and stop transmission.
- Provide optimized care for all patients, especially the seriously ill.
- Minimize the impact of the epidemic on health systems, social services, and economic activity.
Based on the largest cohort of COVID-19 patients, about 40% of patients with COVID-19 may have mild disease, where treatment is mostly symptomatic and does not require inpatient care; about 40% of patients have a moderate disease that may require inpatient care; 15% of patients will have severe disease that requires oxygen therapy or other inpatient interventions, and about 5% have a critical disease that requires mechanical ventilation.[1] However, the evolution of the outbreak in some countries has shown a higher proportion of severe and critical cases and the need to rapidly increase surge capacity to prevent the rapid exhaustion of biomedical supplies and staff. In some countries, doubling rates of cases every 3 days has been observed.[2]
Scenarios of transmission
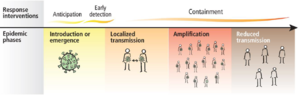
Countries or subnational areas will have to respond rapidly to one or more epidemiological scenarios. Currently, four transmission scenarios are observed:[3]
- Countries with no cases (no cases);
- Countries with one or more cases, imported or locally acquired (sporadic cases);
- Countries experiencing cases clusters in time, geographic location, or common exposure (clusters of cases);
- Countries experiencing larger outbreaks of local transmission (community transmission).
Countries will experience one or more of these situations at the subnational level and must tailor their approach to the local context. For clinical care, six major interventions must be put into place immediately and then scaled up according to epidemiologic scenarios (see Table 3).
Scenario and strategic priorities
Table 1. Key recommendations based on case severity and risk factors, irrespective of transmission scenario
| Case severity, risk factors | Recommendations |
|---|---|
| Mild Moderate with no risk factors (a) | Patient should be instructed to self-isolate and contact COVID-19 information line for advice on testing and referral.
Test suspected COVID-19 cases according to diagnostic strategy. Isolation/ cohorting in:
Self-isolation at home according to WHO guidance. |
| Moderate, with risk factors Severe Critical | Patient should be instructed to self-isolate and call COVID-19 hotline for emergency referral as soon as possible.
Hospitalization for isolation (or cohorting) and inpatient treatment. Test suspect COVID-19 cases according to diagnostic strategy. |
(a) Known risk factors for severe COVID-19: age over 60 years, hypertension, diabetes, cardiovascular disease, chronic respiratory disease, immunocompromising conditions. Note: Probable cases should be retested immediately.
Table 2
| Scenario | Priorities |
|---|---|
| No cases |
|
| Sporadic cases |
|
| Clusters of cases |
|
| Community transmission |
|
Immediate public health interventions
Table 3 Summary of immediate public health interventions, irrespective of transmission scenario
| Topic | Action points |
|---|---|
| Community messaging | Messages should include the following:
|
| Health facility readiness |
|
| Health staff readiness |
|
| Referral system readiness [8] | # Communicate the details of COVID-19 designated facilities to all command and dispatch centres for appropriate destination triage.
|
| Designate COVID-19 treatment areas within health facilities |
|
| Maintain essential health services |
|
Key clinical and IPC activities for different transmission scenarios
Table 4 Key clinical and IPC activities for different transmission scenarios
| No case | Sporadic cases | Clusters of cases | Community transmission | |
|---|---|---|---|---|
| Facility space, including for triage | Usual space. Enhanced screening and triage at all points of first access to the health system. | Dedicated COVID-19 patient care areas within health facility (e.g. infectious disease ward, isolation rooms in emergency or ICU wards). | More patient care areas repurposed for COVID-19 within the health system, especially for severe cases. | Expanded care for severe cases in new hospitals or temporary hospital facilities. |
| Staff | Usual staff.
Train all staff for safe COVID-19 recognition and care. Activate IPC task force. |
Additional staff called in and trained. | Staff extension (supervision of larger number of staff).
Expanded care team model with task shifting or task sharing, and relevant changes in responsibility. |
Make every effort to ensure sufficient staff available. Expanded care team model and additional emergency medical teams (EMTs).4 |
| Supplies | On-hand supplies.
Equip wards for COVID-19 treatment. Identify essential equipment and supplies, including oxygen. Prepare expanded local supply chain. |
Expanded inventory of supplies with detailed protocols for use.
Activate expanded local supply chain.Prepare national supply chain. |
Conservation, adaptation, selected re-use when safe.
Activate contingency planning and procurement for essential equipment and supplies. National supply chain. Prepare expanded supply chain at global level. |
Activate contingency planning should critical equipment be in short supply.
Determine allocation of life- saving resources for HCWs and patients. Activate expanded global supply chain. |
| Standard of care | Usual care with enhanced awareness and recognition of immediate needs for first COVID-19 patients. | Usual care and treatment for all patients, including those with COVID-19. | Identify context-relevant core services. Shift service delivery platforms. Consider reduction in elective patient encounters, including elective surgical procedures. | Mass critical care (e.g. open ICU for cohorted patients). |
| Care areas expansion | No requirements for expansion. | Designate 10 beds per suspected COVID-19 case. | Expand COVID-19 patient- care areas by a factor of 3- 5. | Expand COVID-19 patient care areas by a factor of 5- 8. |
Referral pathways
Screening and triage
Screening: An area in which an individual is evaluated and screened using the case definition; if the person becomes a suspected case, refer to COVID-19 protocol. Isolation: If the case definition is met, the patient should immediately be given a mask and directed to a separate area (an isolation room if available). At least 1 m distance should be kept between suspected patients and other patients.
Triage: Acuity-based triage is the standard method of sorting patients in the medical setting. This is used as the basis for identifying patients who require immediate medical intervention, patients who can safely wait, or patients who may need to be transported to a specific facility based upon their condition. A standard, validated tool should be used to assess for severity of patients and designation to the appropriate part of the facility or the health care system (such as the Integrated Interagency Triage Tool).
Example scenario 1: Mildly ill patient has concerns about having COVID-19. Patient calls COVID-19 hotline for information. Patient is instructed to go for testing at designated site, be evaluated at community centre, or to stay at home in self-isolation (determined by testing strategy and available facility resources).
Example scenario 2: Severely ill patient has concerns about having COVID-19. Patient calls prehospital care service and a basic COVID-19 ambulance is sent for the patient. Patient is transported to facility, screened as suspected COVID-19 patient, and triaged to appropriate level of emergency care based on acuity of disease presentation.
Hub and spoke model (community transmission)
Example scenario: During community transmission, there will be need for multiple COVID-19 treatment areas; a hub and spoke model of referral is recommended.
References
- ↑ Wu Z, McGoogan JM. Characteristics of and Important Lessons From the Coronavirus Disease 2019 (COVID-19) Outbreak in China: Summary of a Report of 72 314 Cases From the Chinese Center for Disease Control and Prevention. JAMA. 2020. doi: 10.1001/jama.2020.2648. [Epub ahead of print]
- ↑ Ministero della Salute. Nuovo coronavirus: Cosa c’è da sapere. http://www.salute.gov.it/portale/documentazione/p6_2_8.jsp?lingua=italiano (accessed 18 March 2020).
- ↑ World Health Organization. Critical preparedness, readiness and response actions for COVID-19.
- ↑ World Health Organization. Emergency Medical Teams Initiative: Guidance and Publications.
- ↑ World Health Organization. Emergency Medical Teams Initiative: Guidance and Publications.
- ↑ World Health Organization. Infection prevention and control during health care when COVID-19 is suspected.
- ↑ World Health Organization. Basic Emergency Care: approach to the acutely ill and injured.
- ↑ Pan American Health Organization. Prehospital Emergency Medical Services Readiness Checklist for COVID-19: Instructive.
- ↑ World Health Organization. Rational use of personal protective equipment for coronavirus diseases (COVID-19).